The main requirement for opening an HSA is having an HSA-eligible health plan, typically a high-deductible health plan (HDHP), Bronze plan or Catastrophic plan, that meets IRS guidelines for the annual deductible and out-of-pocket maximum. To be an eligible individual and qualify for an HSA, the following requirements must be met:
- The individual must have a valid email address, Social Security Number and a primary residence in the United States.
- The individual must be covered by the HSA-eligible health plan on the first day of the month in which they plan to start contributing to their HSA.
- The individual can’t be covered by any other type of health plan, including Medicare Part A or Medicare Part B.
- The individual can’t be covered by TRICARE.
- The individual can’t have used Veterans Administration medical benefits for any non-service-connected disabilities at any time within the past three months (to contribute to an HSA). Note: Title 38 of the United States Code, Section 101(17) defines "non-service-connected" as, with respect to disability, that such disability was not incurred or aggravated in line of duty in the active military, naval, or air service.
- The individual can’t be claimed as a dependent on another person's tax return.
- The individual can’t be covered by a general purpose healthcare Flexible Spending Account (FSA) or Health Reimbursement Account (HRA). Alternative plan designs, such as a limited-purpose FSA or HRA, might be permitted.
- The individual isn’t covered by a general purpose healthcare Flexible Spending Account (FSA) or Health Reimbursement Account (HRA). Alternative plan designs, such as a limited-purpose FSA or HRA, might be permitted.
HDHPs, as well as Bronze and Catastrophic plans, are health plans that satisfy certain requirements for deductibles and out-of-pocket expenses. They typically feature higher deductibles and lower premiums than traditional insurance plans and are the only plan type that can be combined with an HSA. View the IRS guidelines and eligible expenses.
In addition to the HSA-eligible health plan, an individual may have coverage from "permitted insurance," which is coverage related to compensation from workers' compensation, tort liabilities, liabilities relating to ownership or use of property, insurance for a specified disease or illness and insurance that pays a fixed amount per day of hospitalization. Coverage for accidents, disability, dental care, vision care, Direct Primary Care (DPC) arrangements, telehealth services or long-term care does not disqualify an individual from opening an HSA.
No. Each spouse must open a separate HSA. An individual can, however, give their spouse access to their HSA by designating them as an authorized signer on the account.
Anyone may contribute to an HSA on the accountholder’s behalf, as long as they are HSA-eligible and the amount is within the annual IRS contribution limits.
No, as long as they are eligible to contribute. Contributions may be made by the accountholder, or on their behalf, even if they are retired, have no income or their income is less than their contributions.
Yes. The IRS determines the maximum amount that can be contributed to an HSA during the calendar year. View this year's contribution limits.
HSA contributions must be prorated to avoid tax penalties. Below are examples:
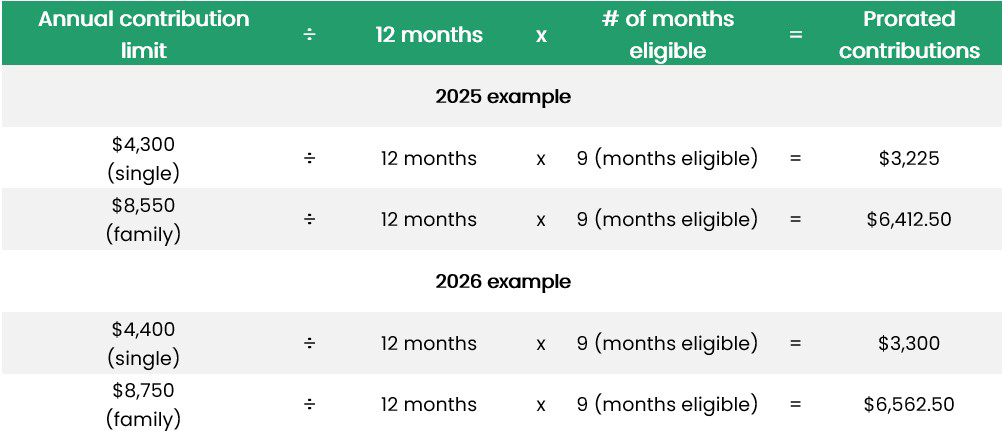
Mid-year Coverage
An individual can contribute the maximum amount for the year if they’re covered by the first day of the last month of the tax year (December 1), and provided they maintain HSA-eligible coverage until December 31 of the following year. This rule can also be applied to $1,000 catch-up contributions for accountholders aged 55 and older.
Health Plan Status Change
If the accountholder begins the year with family coverage and switches to single coverage in July of that year, they are eligible to contribute half of the family coverage contribution maximum and half of the individual coverage contribution maximum.
Yes, yearly contributions should be made by the tax filing deadline, generally April 15 of the following year.
If HSA contributions exceed the IRS contribution limits, the individual must report the excess amount as gross income on their income tax. They will also have to pay additional excise tax on this amount. However, they can remove the excess contributions by submitting an Excess Contribution Removal form to HSA Bank within that tax year.
An individual can pay for a wide range of IRS-qualified medical expenses with their HSA, including many that aren't typically covered by health insurance plans. This includes deductibles, co-insurance, prescriptions, dental and vision care and more. For a complete list of IRS-qualified medical expenses, visit irs.gov or our qualified expenses page.
Generally, health insurance premiums ARE NOT considered IRS-qualified medical expenses, UNLESS they are for:
- Qualified long-term care insurance
- COBRA health care continuation coverage
- Health care coverage while an individual is receiving unemployment compensation
- Direct Primary Care (DPC) arrangements
For individuals over 65, the following premiums ARE considered IRS-qualified medical expenses:
- Medicare Parts A, B, D, Medicare HMA
- Employee portion paid for employer-sponsored health insurance
- Employee portion paid for employer-sponsored retiree health insurance
Yes, as long as the IRS-qualified medical expenses were incurred after the HSA was established, an individual can pay for them or reimburse themselves with HSA funds at any time. They should be sure to keep sufficient records to show that these expenses were not previously paid for by another source or taken as an itemized deduction in any prior tax year.
The HSA accountholder is responsible. So, it's important they keep records of the IRS-qualified medical expenses they pay for with their HSA in order to exclude those dollars from their gross income.
HSA funds that are used to pay for non-IRS-qualified medical expenses are considered part of an individual’s gross income and subject to additional tax.* Exceptions include HSA distributions that are made after an accountholder's death, disability or after they turn 65.
*HSA contributions and earnings aren’t subject to federal taxes and aren’t subject to state taxes in most states. Contact a tax professional for information about your state.
Yes. An individual can transfer or rollover funds from an MSA or HSA with another custodian to their current HSA at HSA Bank. They can transfer funds at any time, but they are limited to one rollover per 12-month period and the rollover must be completed within 60 days. For more information and step-by-step instructions regarding each process, please visit our dedicated transfer/rollover page.
Yes. Money spent on ineligible costs before age 65 is subject to income tax plus a 20% penalty. After turning 65, they won’t pay the penalty, but the distribution will still be subject to income tax.
An individual can use HSA funds to pay for Medicare premiums, including Medicare Part B, which covers outpatient care, and Part D, which covers prescription drugs (most people don't pay premiums for Part A). An individual can't, however, use the funds for premiums for supplemental, or Medigap, policies.
